Welcome to a series of blogs designed to introduce EDS/HSD biology!
Some of my PhD research (supervised by Dr Darius Köster) is soon to be featured on hEDStogether and is going to involve some relatively complicated biology. To make sure everyone is able to understand and engage with this content, we have produced two short blogs to explain our current understanding of EDS/HSD, which should also help to familiarise our readers with some of the more technical terms often used in this field. In this blog, we are going to briefly introduce EDS, and explain how it can affect collagen.
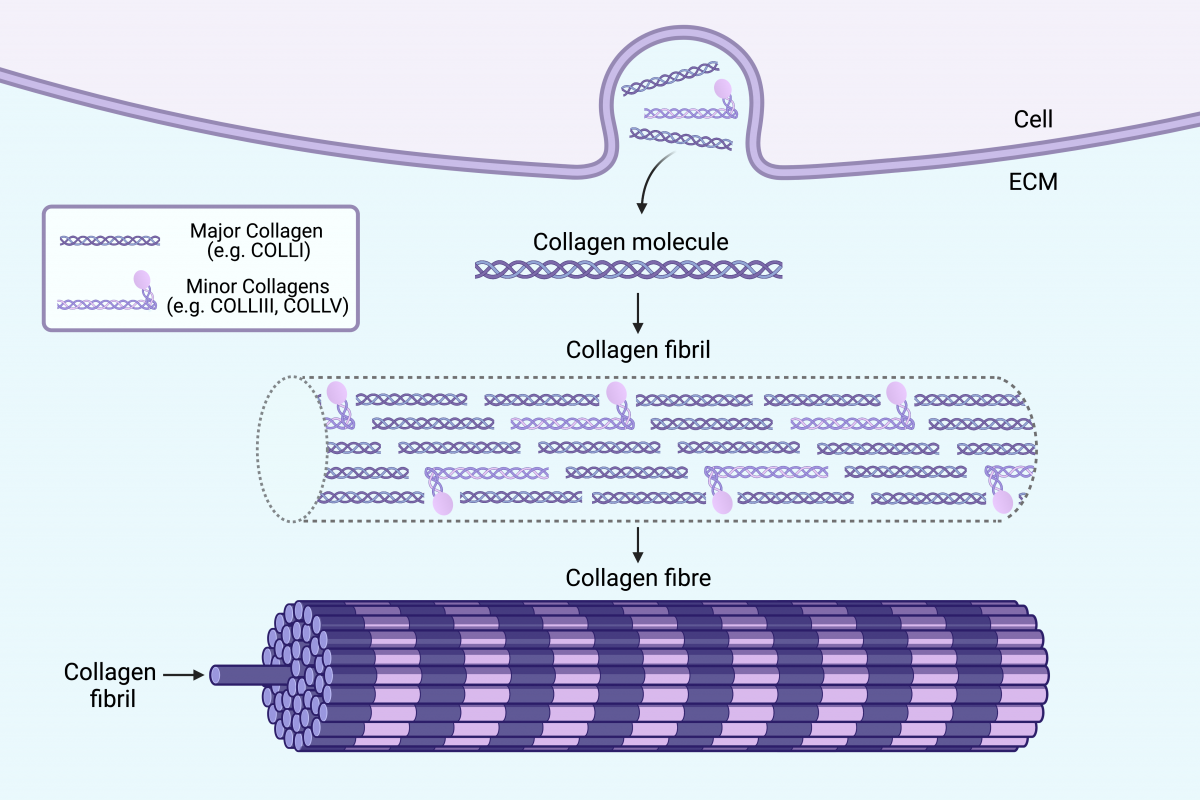
Ehlers-Danlos syndromes (EDS) are 14 conditions that affect the connective tissue. There are three characteristic features that define EDS: joint hypermobility, skin hyperextensibility and tissue fragility. For most of the 14 EDS subtypes, mutations have been found in the genes involved in making collagen. This affects how collagen fibrils and collagen fibres are made (Fig. 1), which is thought to make the connective tissue weak or fragile.
We can see some of these collagen abnormalities when we look at EDS/HSD skin biopsies under the microscope. The first type of abnormality affects the cross-section of the collagen fibril, and gives it a jagged outline instead of a perfectly circular one. This is often called a “flower-like” collagen fibril in the literature. Sometimes, the cross-section of all the collagen fibrils can have different diameters instead of being the same consistent size. The spacing between the collagen fibrils can also be affected, which causes fewer fibrils to be included in the collagen fibre.
The problem with these abnormalities however, is that they are relatively minor and so they don’t provide a full explanation for why the connective tissue is so abnormal in EDS/HSD. These same abnormalities are also seen in people without EDS/HSD, while patients with a confirmed genetic basis for their EDS can sometimes show no collagen abnormalities at all. These therefore, cannot be the specific cause of EDS/HSD.
This leads us to the biggest issues facing EDS/HSD patients today. Without an understanding of exactly how collagen is affected in EDS/HSD, or how it causes the connective tissue to become weak, the diagnostic and treatment options available are limited.
This problem also informs the basis of my PhD research. It is clear, that the collagen fibril analyses are not revealing the answers we need, so could something other than collagen be important for the connective tissue? Are there other aspects of the connective tissue that are relevant to EDS/HSD and need further investigation?
Find out more in blog 2 and future project page about my research. To make sure you don’t miss anything, follow me @SabeehaMalek and @hEDStogether on Twitter!
See you in blog 2!
Sabs
Citation:
Theocharidis, G., & Connelly, JT. (2019). Minor collagens of the skin with not so minor functions. Journal of Anatomy. https://doi.org/10.1111/joa.12584
Angwin, C., Ghali, N., Baker, D., Brady, AF., Pope, FM., Vandersteen, A., Wagner, B., Ferguson, DJP., van Dijk, FS. (2010) Electron microscopy in the diagnosis of Ehlers-Danlos syndromes: correlation with clinical and genetic investigations. British Journal of Dermatology. https://doi.org/10.1111/bjd.18165
Malek, S. & Köster, DV. (2021). The role of cell adhesion and cytoskeleton dynamics in the pathogenesis of the Ehlers-Danlos syndromes and hypermobility spectrum disorders. Frontiers in Cell and Developmental Biology. https://doi.org/10.3389/fcell.2021.649082


